|
Although CD and hysterectomy are hypothesized to make up most of the OB/GYN care in resource-poor areas, the proportion of these procedures compared to overall surgical volume remains unknown. The objective of this systematic review and meta-analysis was to investigate the proportion of OB/GYN to total surgical case volumes in areas lacking surgical care, either in rural high-income countries or in middle- or low-income countries. As a result, current graduates may be “ill prepared” or “uncomfortable” for real-world practice in these challenging environments, , ]. At present, data are lacking to characterize which type of provider performs OB/GYN surgical care in resource-poor areas and how they have been trained. Meta-analysis comparing physicians and nonphysician providers revealed no differences in outcomes however, this conclusion was reached with low confidence because there was a paucity of studies that could be included. Middle- and low-income countries have created a variety of programs that train nurses and nonphysician providers with a variety of titles, such as “assistant medical officers” or “clinical officers”, to perform CD, ,, , ]. The American College of Surgeons, as well as Canadian and Australian initiatives, has developed training programs for general surgeons, family medicine physicians, and midwives to provide life-saving OB/GYN skills in rural areas of high-income countries, ,, ,, ]. In resource-poor areas, physicians and nonphysicians alike address surgical burden in resource poor areas. Despite controversy as to which surgical procedures can be safely performed in rural hospitals, there has been consensus that emergency OB/GYN care must be available in rural facilities in high- and low-income countries alike, , ]. Hospitals with lower birth volumes (< 240 births per year) are more likely to have general surgeons and family physicians attending deliveries than an obstetrician or a midwife. In the United States, estimates reveal that rural surgeons perform up to 66%–71% of OB/GYN inpatient procedures, , ], which make up 27% of the surgeon's overall caseload. In contrast to areas with an abundance of surgical specialists, general surgeons have historically provided OB/GYN care where full-time obstetricians or gynecologists do not exist. A detailed picture of which obstetric or gynecological procedures are needed in these communities remains unclear. 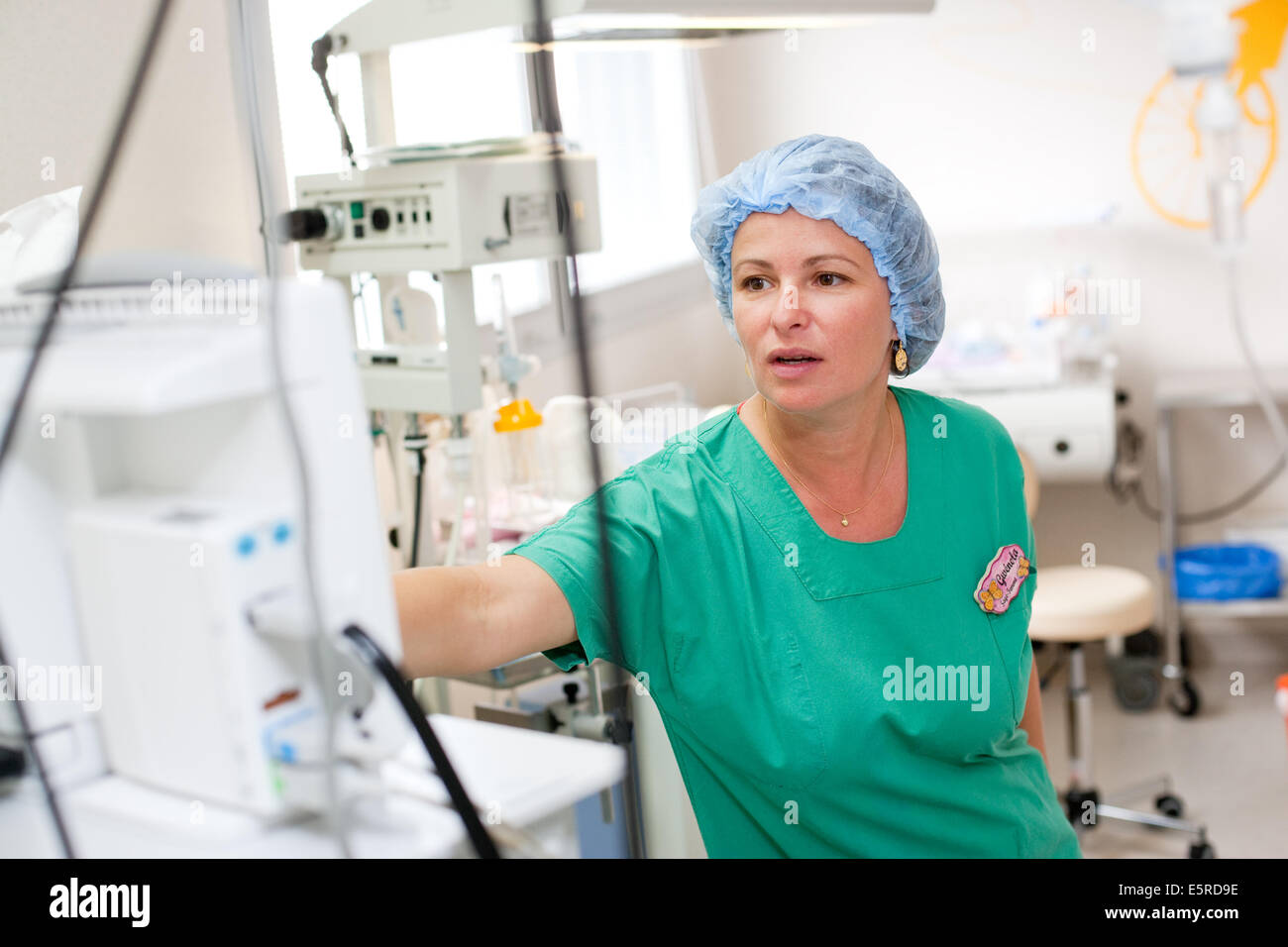
Other procedures include reduction of ovarian torsion, treatment of ectopic pregnancy, ureteral injury or ureteral obstruction, as well as many other different obstetric procedures. Obstetric and gynecologic (OB/GYN) surgical procedures, such as cesarean delivery (CD) and hysterectomy, are proposed to represent a large part of surgical burden in resource-poor areas. 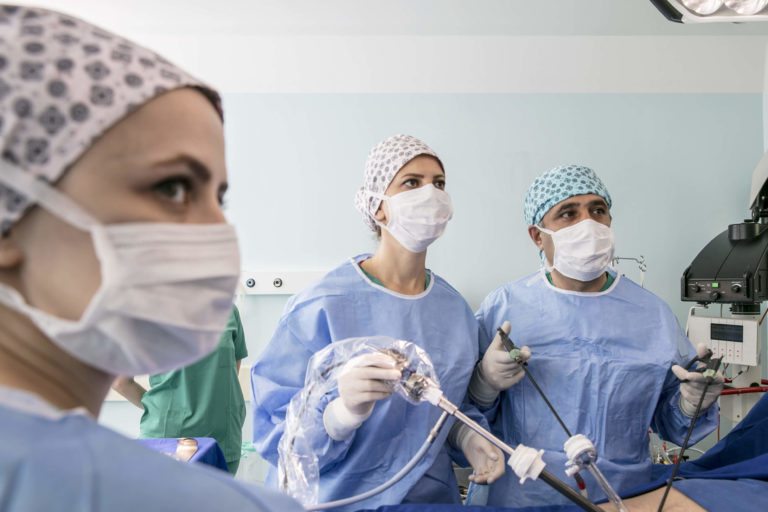
The call for broadly trained surgical providers to serve in “surgical deserts” has gained recognition on a global scale. Improved surgical care in low- and middle-income countries remains a primary focus of the Millennium Development Goals of the World Health Organization (WHO) and the Lancet Commission on Global Surgery, which includes strategy for “universal health care” that is also needed for surgical services within rural developed countries. Surgical care in resource-poor areas may be more cost-effective, however, than other basic health provisions. 
The poorest third of the world's population receives only 3.5% of the world's surgical procedures.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
